Medical Research
A New Chapter in Vision Restoration By Rebuilding Retinal Ganglion Cells
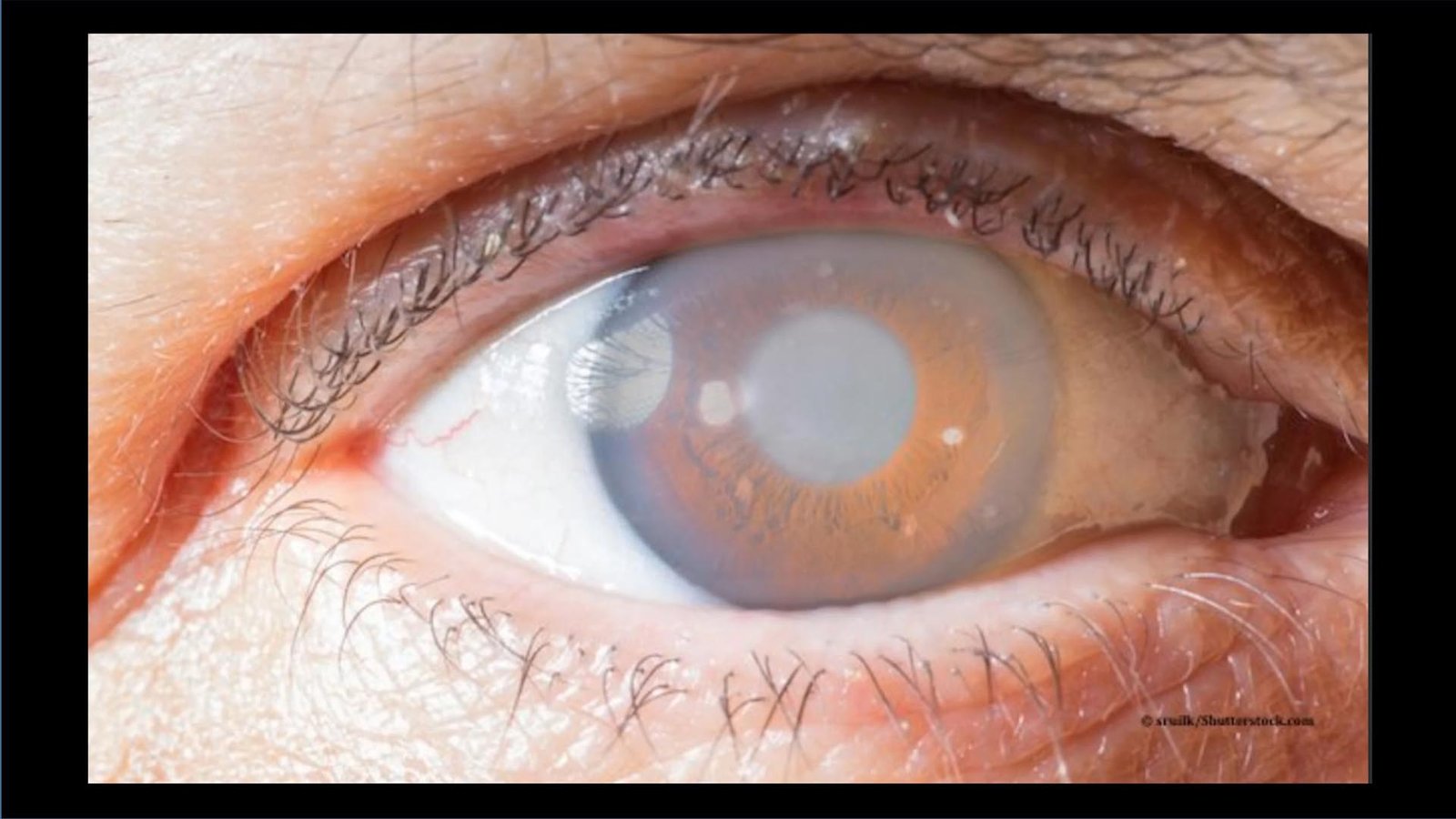
Harvard’s Stem Cell Strategy for Vision Restoration
In a groundbreaking study led by Harvard Medical School researchers at the Schepens Eye Research Institute, a potential game-changer in the fight against glaucoma has emerged. Glaucoma, a leading cause of blindness worldwide, poses a significant challenge as there are currently no effective treatments to reverse vision loss caused by the death of retinal ganglion cells (RGCs).
Glaucoma, a sneaky eye condition, can silently damage your optic nerve, a crucial component for vision. Typically, it occurs when fluid accumulates in the front part of your eye, leading to increased eye pressure and optic nerve damage.
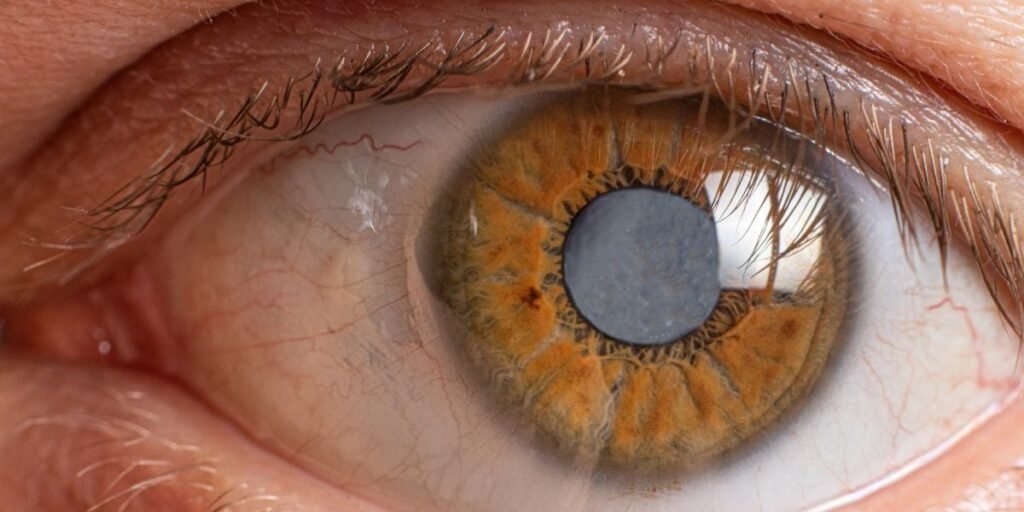
Unpacking the Causes of Glaucoma Your eye produces a fluid called aqueous humor. Ideally, the same amount should flow in and out, maintaining stable intraocular pressure (IOP). However, if the drainage angle isn’t working well, fluid builds up, causing pressure to rise and damaging the optic nerve.
Types of Glaucoma There are two major types:
- Open-angle glaucoma
- Develops gradually.
- Causes painless pressure buildup, initially with no vision changes.
- Regular eye exams are crucial for early detection.
- Angle-closure glaucoma
- Iris is close to the drainage angle.
- Can lead to an acute attack, requiring immediate attention.
- Symptoms include blurry vision, severe eye pain, headaches, and nausea.
Recognizing Glaucoma Symptoms
- Open-angle glaucoma: Sneaky and symptom-free until peripheral vision develops blind spots.
- Angle-closure glaucoma: Risky, with no warning signs. Attack symptoms include severe eye pain, redness, blurred vision, and nausea.
Who’s at Risk for Glaucoma? Some factors increase the risk
Age over 40
- Family history of glaucoma
- African, Hispanic, or Asian heritage
- High eye pressure
- Eye injuries or use of long-term steroid medications
- Other health issues like diabetes or high blood pressure
Diagnosing Glaucoma The only surefire way is a comprehensive eye exam, not just a pressure check. Your ophthalmologist will assess eye pressure, drainage angle, optic nerve health, peripheral vision, and more..

Unfortunately, glaucoma damage is irreversible, but treatments can prevent further harm. Options include medication, laser surgery, and operating room procedures.
Medication Eyedrop medicines control glaucoma by reducing eye pressure. Side effects may include stinging, redness, or changes in vision.
Laser Surgery
- Trabeculoplasty: Enhances drainage angle function for open-angle glaucoma.
- Iridotomy: Creates a small hole in the iris for angle-closure glaucoma.
Operating Room Surgery
- Trabeculectomy Creates a flap to allow fluid drainage.
- Glaucoma Drainage Devices Implants a tube for fluid collection.
- Cataract Surgery Removes the eye’s natural lens to alleviate pressure in some cases.
Remember, early detection and treatment can be your best defense against the “silent thief of sight.”
However, the researchers might have found a promising avenue for treatment using a multidisciplinary approach.
The study, published on November 6 in the prestigious journal PNAS, showcased a remarkable strategy involving the transformation of blood stem cells into functional retinal ganglion cells. These RGCs, responsible for transmitting visual information from the eye to the brain, were successfully created in the lab. The key innovation here was altering the microenvironment in the eye to facilitate the conversion of blood stem cells into RGCs capable of migrating and surviving in the retina.
Traditionally, cell transplants have been explored as a potential treatment for replacing RGCs. However, this method is still in the research and development stage and faces significant limitations. One major challenge is that donor cells often remain at the injection site and fail to migrate to the areas where they are most needed in the retina. This limitation prompted the researchers to seek a more precise and effective approach to repopulating these crucial cells.
Enter the world of chemokines, signaling molecules that play a vital role in guiding the movement and integration of cells. The research team took a big data approach, examining hundreds of such molecules and receptors. In this extensive exploration, they identified 12 chemokines that were unique to RGCs. Among them, stromal-derived factor 1 stood out as the most effective molecule for both migration and transplantation of the newly created RGCs.

Senior author Petr Baranov, an assistant professor of ophthalmology at Schepens, expressed enthusiasm about the potential of this approach. He highlighted the use of chemokines as a promising method to guide donor cell movement and integration, presenting a hopeful avenue for restoring vision in glaucoma patients. The excitement stems from the successful application of these techniques in the adult mouse retina, raising the possibility of future applications in the human retina.
This innovative method could revolutionize cell replacement therapy, providing a more targeted and efficient way to repopulate retinal ganglion cells. It’s not just about treating glaucoma; the implications extend to potential applications in addressing other neurodegenerative conditions. The researchers’ journey involved collaboration across diverse fields, bringing together experts in ophthalmology, bioengineering, and bioinformatics.

Jonathan R. Soucy, the lead study author and a bioengineer from Baranov’s lab at Mass Eye and Ear, played a crucial role in the study. Alongside lead bioinformatician Emil Kriukov, the team utilized their unique expertise to develop novel techniques for modifying the local environment to guide cell behavior.
RAED MORE MEDICAL RESEARCHED ARTICLES Regenerative Surgery A Comprehensive Innovation by Stem Cells in Face and Eye Transplantation
In conclusion, this study opens up a promising avenue for treating glaucoma and, potentially, other neurodegenerative conditions. The use of chemokines to guide the movement and integration of donor cells represents a significant leap forward in the quest to restore vision. As the research progresses, the hope is that these findings will pave the way for future breakthroughs in the field of regenerative medicine, offering new hope to individuals facing vision loss due to conditions like glaucoma
Medical Sciences
Nanodrones Against Cancer,UNIST’s Innovation Marks a New Era in Treatment

Game-Changer in Cancer Research: UNIST’s Nanodrones Take the Spotlight
In the realm of groundbreaking cancer treatment breakthroughs, the spotlight is now on the Ulsan National Institute of Science and Technology (UNIST), where a dynamic team of researchers has unveiled a potential game-changer. Imagine a world where tiny nanodrones, aptly named NK cell-engaging nanodrones (NKeNDs), take center stage in the fight against cancer.
RELATED ARTICLE New revolutionary nanodrones enable targeted cancer treatment
Led by the innovative minds of Professors Sebyung Kang and Sung Ho Park from the Department of Biological Sciences, this team has cracked the code to revolutionize cancer treatment. These nanodrones, far from the futuristic sci-fi portrayals, are engineered to specifically target and obliterate cancer cells, marking a significant leap forward in the battle against this relentless disease.

At the heart of this breakthrough lies the ability of these nanodrones to engage natural killer (NK) cells, the body’s frontline soldiers against cancer. What sets the NKeNDs apart is their precision – think of them as nanoscale guided missiles homing in on cancer cells with unparalleled accuracy. The secret sauce involves utilizing AaLS protein cage nanoparticles as the foundation for these nanodrones, incorporating specific cancer-targeting and NK cell-recruiting ligands, aptly named HER2 @NKeND and EGFR@NKeND.
Lab tests have showcased the remarkable ability of these nanodrones to selectively bind to various types of cancer cells while rallying NK cells to mount a defense against the invaders. The real breakthrough emerged during mice trials, where administering HER2 @NKeNDs alongside human immune cells resulted in a significant slowdown in tumor growth, all without adverse effects.

Professor Kang Se-byung, brimming with excitement, highlighted the potential for customizing treatments for different cancers using these NK cell delivery nanodrones. It’s not merely about targeting cancer cells; it’s about doing so with surgical precision, minimizing collateral damage and maximizing the impact of the body’s immune system.
MORE LATEST ARTICLE Brain Clot Revolution, Vortex Ultrasound Tornado in Brain Health
This groundbreaking study, published in Nano Today, marks a pivotal moment in scientific progress. With the support of various institutions dedicated to advancing knowledge, the door to a new era in cancer treatment swings wide open. Nanodrones may just be the superheroes we’ve been yearning for, offering hope and resilience in the face of one of humanity’s most formidable adversaries. As we raise a toast to science and innovation, the journey towards conquering cancer takes a remarkable leap forward. Cheers to the heroes of the microscopic world.
Medical Sciences
Revolutionizing Hypertension Treatment, Zilebesiran’s Promise in Cardiovascular Health

Zilebesiran’s Pioneering Role in Hypertension Care
In the dynamic realm of cardiovascular research in 2023, the American Heart Association (AHA) has spotlighted groundbreaking advances that promise to reshape the landscape of heart health. Researchers have delved into various dimensions, from innovative drug therapies to cutting-edge procedures, offering hope for improved prevention and treatment of cardiovascular diseases.
RELATED ARTICLE AHA names top advances in cardiovascular disease research for 2023

Brief Introduction about zilebesiran
A solitary administration of the experimental drug zilebesiran demonstrated both safety and efficacy in reducing systolic blood pressure in individuals with mild-to-moderate high blood pressure for a duration of up to six months. This information, disclosed in the Phase 2 segment of the KARDIA study, was presented as late-breaking scientific findings during the American Heart Association’s Scientific Sessions 2023. The conference, held from November 11 to 13 in Philadelphia, serves as a leading global platform for the exchange of cutting-edge scientific developments, research insights, and updates on evidence-based clinical practices in the field of cardiovascular science.
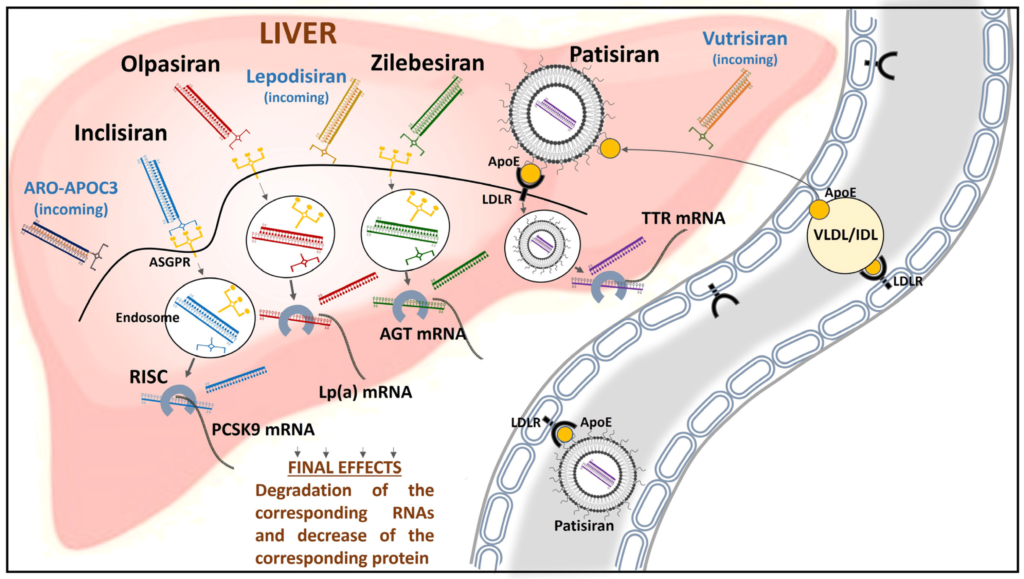
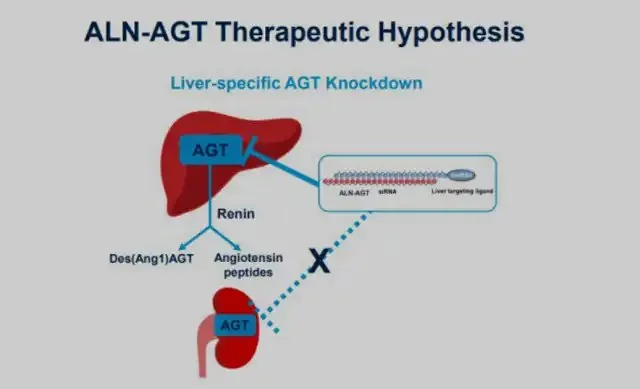
Zilebesiran functions as an investigational RNA interference agent designed to target angiotensinogen (AGT), a hormone primarily produced in the liver that plays a significant role in the regulation of blood pressure.
RELATED INFORMATION New drug zilebesiran effectively lowers blood pressure for six months, study finds
One notable stride involves a novel drug targeting hypertension. In this arena, Zilebesiran, an investigational drug, has emerged as a potential game-changer. In a phase I study involving 107 participants aged 65 and older with high blood pressure, the drug exhibited promise by reducing blood pressure measurements over an eight-week period. The study demonstrated efficacy, even with a single dose, offering potential advantages in terms of accessibility to care and adherence to long-term drug regimens. Moreover, the drug’s impact extended beyond hypertension, sparking excitement about its potential therapeutic applications for kidney and heart diseases.
Another significant breakthrough lies in the realm of stroke treatment. Endovascular thrombectomy, a minimally invasive procedure to remove blood clots causing strokes, has traditionally been applied to medium-sized strokes. However, new studies from various regions, including China, North America, Europe, Australia, and New Zealand, have presented compelling evidence that this procedure could benefit individuals with larger, more severe strokes. The trials, published in renowned journals such as the New England Journal of Medicine and The Lancet, underscored the procedure’s superiority in improving functional independence and reducing disabilities in severe stroke patients.

Advancements in imaging techniques have also taken center stage, particularly in guiding stent placement for individuals with complex coronary lesions. While angiography remains the standard for guiding stent placement, intravascular imaging, including techniques like optical coherence tomography (OCT), has showcased its potential. Studies such as ILUMIEN IV and OCTOBER compared OCT-guided percutaneous coronary intervention (PCI) to angiography-guided PCI, revealing that OCT guidance resulted in a larger minimum stent area, suggesting improved outcomes in complex cases.
The intersection of atrial fibrillation (AFib) and stroke treatment has seen intriguing developments. A study published in the New England Journal of Medicine challenges the conventional timeline for initiating anticoagulant treatment in AFib patients following a stroke. Contrary to current practice guidelines, early initiation of Direct-Acting Oral Anticoagulants (DOACs) within 48 hours of a minor or moderate stroke, and on day six or seven following a major stroke, demonstrated promising results. The study suggests that CT or MRI scans could offer more precise insights into stroke severity, aiding in identifying individuals who could benefit from earlier DOAC use.
Furthermore, the realm of cardiovascular health has expanded its reach to individuals without diabetes. Semaglutide, a medication primarily approved for long-term weight management in individuals with obesity, has exhibited potential cardiovascular benefits. Studies indicated that it not only lowered the risk of heart problems in people with diabetes but also showcased effectiveness in reducing heart failure-related symptoms and cardiovascular-related death in overweight and obese individuals without diabetes.
The AHA has also emphasized the role of social determinants of health in cardiovascular disparities. Research linking cardiovascular death rates to income status, access to healthy foods, and housing highlights the need to address these social factors for effective cardiovascular disease prevention and management.
On a broader scale, the AHA has taken a holistic approach with the introduction of the cardiovascular-kidney-metabolic (CKM) syndrome. This syndrome, encompassing the intricate interconnections between obesity, chronic kidney disease, diabetes, and cardiovascular disease, has prompted the development of a new risk calculator. The American Heart Association PREVENT risk calculator now estimates 10- and 30-year risks for heart attacks, strokes, and heart failure, incorporating measures of cardiovascular, kidney, and metabolic health, along with considerations for social determinants of health.
READ MORE SCIENTIFIC ARTICLE Brain Clot Revolution, Vortex Ultrasound Tornado in Brain Health
Lastly, the spotlight extends to the treatment of peripheral arterial disease (PAD), particularly chronic limb-threatening ischemia. Studies such as BASIL-2 and BEST-CLI have compared the effectiveness of surgical bypass to endovascular therapies, offering insights into optimal intervention choices for improved outcomes.
In essence, the cardiovascular research landscape of 2023 paints a vivid picture of innovation, ranging from novel drug therapies to sophisticated procedures and holistic risk assessment tools. As we navigate this evolving landscape, the promise of enhanced prevention, treatment, and overall cardiovascular health stands as a beacon of hope for individuals worldwide.
Medical Sciences
Decoding Waardenburg Syndrome,Genetic Aspects and Clinical Nuances of Waardenburg Syndrome

Understanding Waardenburg Syndrome: Genetic Aspects and Clinical Insights
Introduction
Waardenburg syndrome stands as a rare genetic disorder renowned for its distinctive features involving sensorineural hearing loss and pigmentary abnormalities affecting the hair, skin, and eyes. Named after the Dutch ophthalmologist Petrus Johannes Waardenburg, who first observed the correlation between deafness and heterochromia iridis, this syndrome has been a subject of keen medical interest.
RESOURCED ARTICLE Waardenburg syndrome
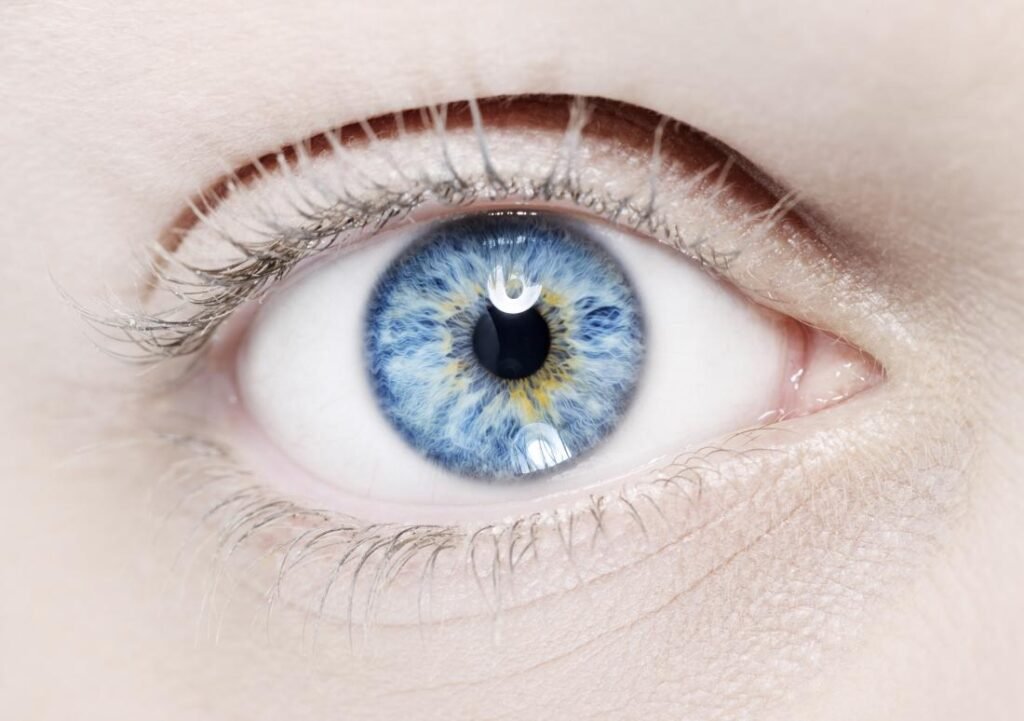
Demographics and Frequency: Waardenburg syndrome does not discriminate; it affects both males and females equally and can manifest across all races. With a population frequency of approximately 1 in 40,000, it contributes to 2–5% of all cases of congenital deafness.
Genetic Basis: This neurocristopathy arises from gene mutations affecting neural crest differentiation during embryonic development. Various genes play pivotal roles, and their mutations give rise to different types of Waardenburg syndrome. Noteworthy genes include:
- PAX3 (Chromosome 2q): Implicated in WS1 and WS3.
- MITF (Chromosome 3p): Associated with WS2A.
- Chromosomes 1p, 8p, 8q, 13q, 20q, and 22q: Linked to WS2B, WS2C, WS2D, WS4A, WS4B, and WS4C, respectively.
The mutations encompass various types such as insertions, deletions, frameshifts, splice alterations, missense, or nonsense mutations. Interestingly, most types of Waardenburg syndrome follow an autosomal dominant inheritance pattern, meaning that one affected gene passed on to a child is sufficient for them to exhibit the syndrome. However, complexities arise with genes like EDN3 or EDNRB, which generally follow autosomal recessive patterns.
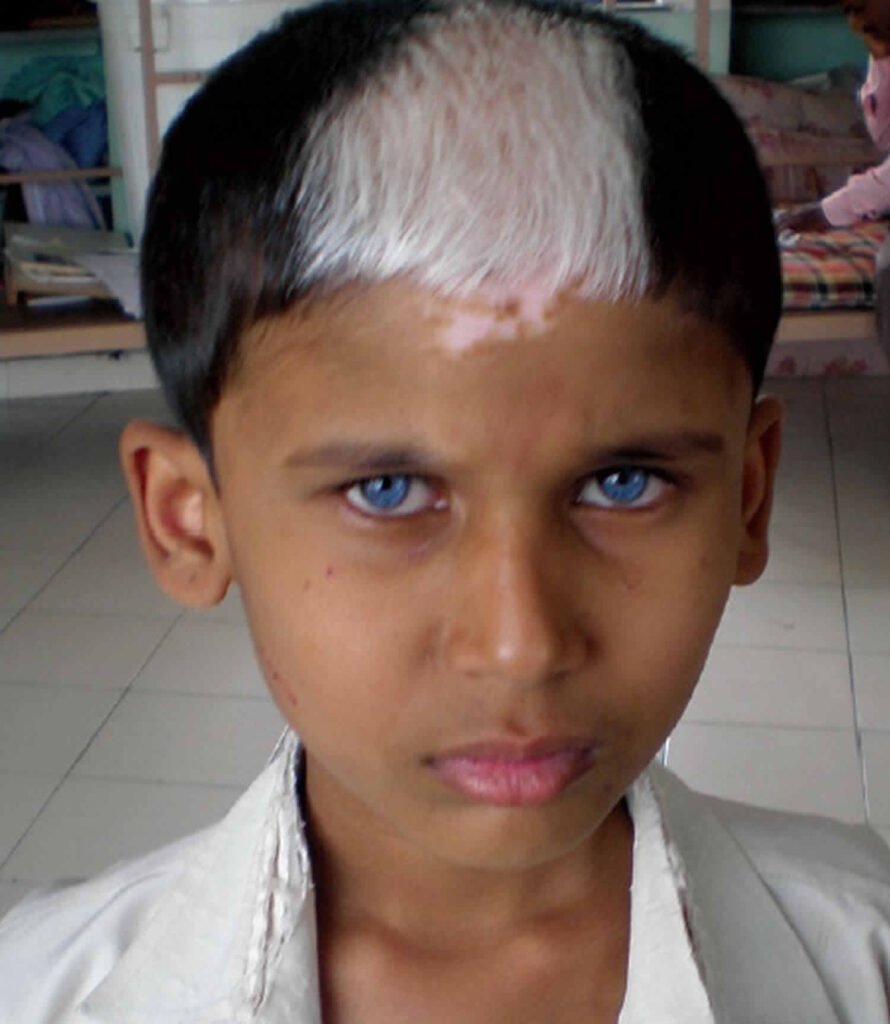
Clinical Features: Waardenburg syndrome manifests early in life, and its diagnosis can be challenging due to the subtlety of clinical signs. Major types (Type 1-4) display distinct features:
- Type 1: Most common, characterized by sensorineural deafness, distinct facial features, white skin patches, and pigmentary abnormalities in the eyes.
- Type 2: Similar to Type 1 but lacks abnormalities in the inner canthi.
- Type 3 (Klein-Waardenburg syndrome): Includes musculoskeletal abnormalities.
- Type 4 (Shah-Waardenburg syndrome): Similar to Type 2 but with the addition of Hirschsprung syndrome.
Diagnosis: The diagnosis of Waardenburg syndrome relies on clinical features, with major criteria encompassing sensorineural deafness, iris pigmentary abnormalities, and hair pigmentation anomalies. Minor criteria include features like unpigmented skin patches, synophrys, and premature greying of scalp hair. The W index, calculated based on canthal distances, aids in identifying dystopia canthorum. Genetic sequencing, particularly of the PAX3 gene, can provide a definitive diagnosis and guide genetic counseling.

Treatment and Management: As of now, there is no curative treatment for Waardenburg syndrome due to its genetic nature. Genetic counseling is crucial for affected individuals contemplating starting a family. Regular audiology examinations are recommended for managing deafness, and those with Hirschsprung syndrome may require surgery. Sun protection is emphasized for areas with unpigmented skin patches.
Outlook: Waardenburg syndrome presents stable clinical features throughout life, and individuals can expect a normal life expectancy. Although the syndrome poses challenges, advancements in genetic understanding have paved the way for improved diagnostics and counseling, offering individuals and families affected by Waardenburg syndrome a clearer path forward.
READ MORE INTERESTING ARTICLE Cortex Chronicles, Paul G. Allen’s Institute Explores the Study on Visual Masking in Bioscience
In conclusion, the intricate genetic landscape of Waardenburg syndrome underscores the importance of ongoing research and medical advancements in unraveling the complexities of this rare disorder. As we delve deeper into the genetic intricacies, our ability to diagnose, manage, and provide support for individuals with Waardenburg syndrome continues to evolve.
-
 Medical Sciences8 months ago
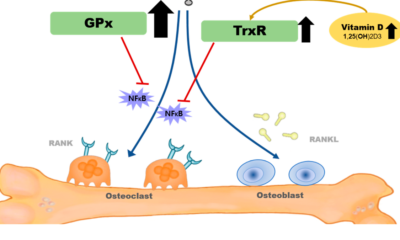
Medical Sciences8 months agoSelenium Nanoparticles Redefining Postmenopausal Osteoporosis Treatment with a Novel Approach
-

 Medical Sciences8 months ago
Medical Sciences8 months agoTransforming Heart Failure Care: Unveiling Abbott’s ARIES Trial Breakthrough with Aspirin-Free HeartMate 3
-

 Medical Sciences7 months ago
Medical Sciences7 months agoNanodrones Against Cancer,UNIST’s Innovation Marks a New Era in Treatment
-
 Medical Sciences8 months ago
Medical Sciences8 months agoGeriatric Care in the Face of Non-ST Elevated Myocardial Infarction and Acute Coronary Syndrome
-

 Blog8 months ago
Blog8 months agoUK’s Milestone In Genetic Medicine,CRISPR Therapy Treating Sickle-Cell Disease and β-Thalassaemia
-

 Blog8 months ago
Blog8 months agoCutting-Edge Diagnostic Technology Handheld Device for Alzheimer’s and Parkinson’s Diseases
-
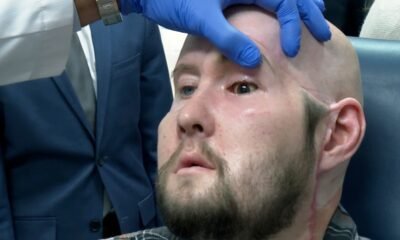
 Medical Sciences8 months ago
Medical Sciences8 months agoRegenerative Surgery A Comprehensive Innovation by Stem Cells in Face and Eye Transplantation
-
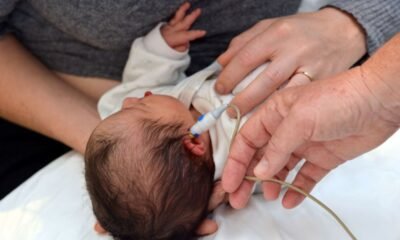
 Blog8 months ago
Blog8 months agoNewborn Hearing Screening Can Improve Reading Proficiency Skills
